DEFENCE: Researchers say boosting the body’s own anti-inflammatory ‘brakes’ may offer a safer way to ease chronic inflammation without suppressing immunity…
By Own Correspondent
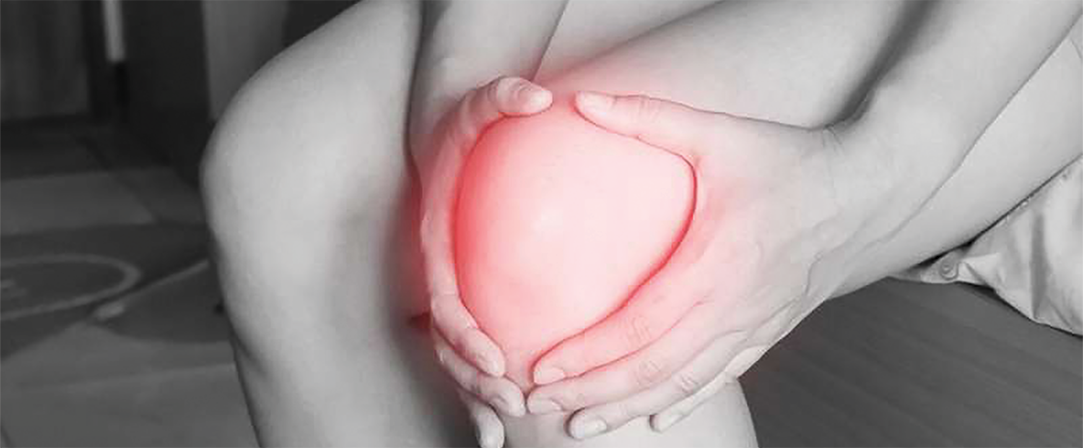
Researchers at University College London (UCL) have uncovered a key biological mechanism that helps the body shut down inflammation — a discovery that could pave the way for new treatments for chronic inflammatory diseases such as arthritis, heart disease and diabetes.
Inflammation is the immune system’s frontline response to infection or injury. But when it fails to switch off properly, it can become harmful, driving tissue damage and long-term illness. Until now, scientists have not fully understood how the body transitions from “fight mode” into healing.
In a study published in Nature Communications, UCL researchers found that epoxy-oxylipins — tiny fat-derived molecules produced naturally in the body — act as immune “brakes”. They limit the expansion of intermediate monocytes, a type of immune cell associated with chronic inflammation ==and disease progression.
To test the mechanism in humans, researchers recruited healthy volunteers and triggered a brief inflammatory response by injecting a small amount of UV-killed E. coli bacteria into the forearm. This produced typical short-term inflammation symptoms, including pain, redness, heat and swelling — similar to what occurs during infection or injury.
Participants were divided into two groups:
• Prophylactic group (preventative approach): Volunteers received treatment two hours before inflammation began.
• Therapeutic group (real-world treatment approach): Volunteers received treatment four hours after inflammation started.
Each group included 24 volunteers, split equally between those given the active drug and those given a placebo. Drug boosts protective molecules and speeds pain recovery
At different stages, volunteers received GSK2256294, a drug that blocks an enzyme known as soluble epoxide hydrolase (sEH). This enzyme normally breaks down epoxy-oxylipins. By blocking it, researchers were able to raise epoxy-oxylipin levels in the body.
Interestingly, the treatment did not significantly reduce visible signs such as redness and swelling — suggesting its most meaningful effects may occur at the cellular and pain-response level, rather than in external symptoms.
Further analysis pinpointed one epoxy-oxylipin in particular — 12,13-EpOME — as a major driver of the inflammation “switch-off” process. It works by shutting down a signalling pathway involving a protein called p38 MAPK, which plays a role in transforming immune cells into inflammatory intermediate monocytes.
This mechanism was confirmed through lab tests and through comparisons with volunteers given a separate drug that blocks the p38 pathway.
First author Olivia Bracken from UCL’s Department of Aging, Rheumatology and Regenerative Medicine said the discovery reveals a natural pathway that helps the body prevent harmful immune overactivity.
“Our findings reveal a natural pathway that limits harmful immune cell expansion and helps calm inflammation more quickly,” Bracken said. “Targeting this mechanism could lead to safer treatments that restore immune balance without suppressing overall immunity.”
Corresponding author Professor Derek Gilroy from UCL’s Division of Medicine described the research as the first to map epoxy-oxylipin activity in humans during inflammation.
“By boosting these protective fat molecules, we could design safer treatments for diseases driven by chronic inflammation,” he said, adding that the study used a drug already suitable for human use and potentially ready to be repurposed for inflammatory flare-ups.
Next steps
The researchers say the findings open the door to clinical trials testing sEH inhibitors for conditions such as rheumatoid arthritis and cardiovascular disease.
Health Briefs
Afternoon naps can clear brain
Even a short afternoon nap can help the brain recover and improve its ability to learn.
In a study published on January 22, 2026, in the journal NeuroImage, researchers at the Medical Centre–University of Freiburg (Germany), Geneva University Hospitals (HUG) and University of Geneva (UNIGE), show that even a nap is enough to reorganise connections between nerve cells so that new information can be stored more effectively.
Until now, these effects were only known to occur after a full night’s sleep. The new study shows that a short sleep period can relieve the brain and put it back into a state of readiness to learn—a process that could be particularly beneficial for situations with a high work load.
“Our results suggest that even short periods of sleep enhance the brain’s capacity to encode new information,” says study leader Prof Christoph Nissen, who performed the study during his time as medical director of the sleep centre at the Department of Psychiatry and Psychotherapy at the Medical Centre–University of Freiburg, Germany.
The brain is constantly active during the day: New impressions, thoughts, and information are processed, strengthening the connections between nerve cells (synapses). These strengthened synaptic connections are an important neural basis for learning processes. However, they also lead to saturation, so that the brain’s ability to learn further decreases over time. Sleep helps to regulate this excessive activity again—without losing important information. – Science X
Grandparenting Good for the Brain
WASHINGTON – Helping to care for grandchildren may serve as a buffer against cognitive decline in older adults, according to research published by the American Psychological Association.
“Many grandparents provide regular care for their grandchildren – care that supports families and society more broadly,” said lead researcher Flavia Chereches, of Tilburg University in the Netherlands.
“An open question, however, is whether caregiving for grandchildren may also benefit grandparents themselves. In this research, we wanted to see if providing grandchild care might benefit grandparents’ health, potentially slowing down cognitive decline.”
The research was published in the journal Psychology and Aging.
To study this, Chereches and her colleagues examined data from 2 887 grandparents (all older than age 50, with a mean age of 67). The survey asked whether participants had provided care for a grandchild at any point in the past year.
Overall, the researchers found that grandparents who provided childcare scored higher on tests of both memory and verbal fluency compared with those who didn’t, even after adjusting for age, health and other factors. This held true regardless of the frequency and type of care the grandparents provided.
The researchers also found that grandmothers who provided care saw less decline on cognitive tests over the course of the study compared with those who didn’t.
“More research is needed to replicate these findings, yet, if there are benefits associated with caregiving for grandparents, they might not depend on how often care is provided, or on the specific activities done with grandchildren, but rather on the broader experience of being involved with caregiving,” said Chereches. – Newswise
Black Women, Breast Cancer, Ultra-Processed Foods
A new study has found that Black women with breast cancer who consume high levels of ultra-processed foods face significantly worse survival outcomes, highlighting diet as a potentially modifiable risk factor after diagnosis.
Research led by scientists at Rutgers University-New Brunswick and the Rutgers Cancer Institute shows that women who ate the most ultra-processed foods before diagnosis were 36–40% more likely to die from breast cancer or any cause than those with the lowest intake. The study was published in eClinicalMedicine.
The researchers followed 1 733 Black women diagnosed with breast cancer in New Jersey between 2005 and 2019 as part of the Women’s Circle of Health Follow-Up Study. Women in the highest intake group consumed more than eight servings of ultra-processed foods a day, compared with fewer than three servings among those with the lowest intake.
Ultra-processed foods include sodas, processed meats, sweets, salty snacks and fast foods, which now make up as much as 60% of calories in the typical U.S. diet. Processed meats were identified as the strongest contributor to poorer outcomes.
The findings align with international research, including studies from the UK Biobank, suggesting the biological mechanisms involved are not race-specific. Researchers say reducing processed meat consumption and returning to home-cooked meals could improve long-term health for breast cancer survivors. – Newswise